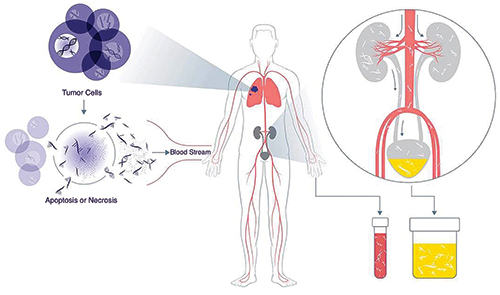
Oncology has risen to the forefront of genomic profiling, which is being used to identify actionable driver mutations and other markers. These markers can help clinicians design therapies and monitor patient responses, and they may be revealed by means of next-generation sequencing (NGS), a catch-all term describing massive parallel sequencing technologies generating gigabases of data.
NGS is already established as a research platform, and it is rapidly gaining acceptance as a clinical platform—at least as far as technical and scientific matters are concerned. Administratively and practically, however, NGS still faces barriers to adoption as a clinical tool. These include regulation, incorporation in clinical guidelines (NCCN, ASCO, etc.), reimbursement, and physician and patient education.
Accordingly, if NGS is to be fully embraced by the clinic, and if the potential for personalized oncology is to be realized, interested parties will have to cooperate and build a sense of shared commitment—at least, that was the sentiment expressed by several of the presenters at the Personalized Medicine World Conference, which was held recently in Mountain View, CA.
For the rest of the story, click here.






![AI Algorithm Could Reduce Breast Cancer Mammogram False Positive Rate The primary goal of the Paradigm Registry is to accelerate tumor profiling based on disease biology. [iStock/LilliDay]](https://www.insideprecisionmedicine.com/wp-content/uploads/2019/01/307-218x150.jpeg)